Restorative Care
Topics on this page
Fillings
Newer dental fillings include ceramic and plastic compounds that mimic the appearance of natural teeth. These compounds are called composite resins.
There are two different kinds of fillings: direct and indirect. Direct fillings are fillings placed into a prepared cavity in a single visit. They include glass ionomers, resin ionomers, and composite (resin) fillings. Indirect fillings generally require two or more visits. They include inlays, onlays, and veneers. They are used when a tooth has too much damage to support a filling but not enough to necessitate a crown.
Dentures
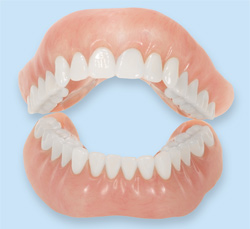 Dentures are natural-looking replacement teeth that are removable. There are two types of dentures: full and partial. Full dentures are given to patients when all of the natural teeth have been removed. Partial dentures are attached to a metal frame that is connected to your natural teeth and are used to fill in where permanent teeth have been removed. Just like natural teeth, dentures need to be properly cared for. Use a gentle cleanser to brush your dentures, always keep them moist when they’re not in use, and be sure to keep your tongue and gums clean as well.
Dentures are natural-looking replacement teeth that are removable. There are two types of dentures: full and partial. Full dentures are given to patients when all of the natural teeth have been removed. Partial dentures are attached to a metal frame that is connected to your natural teeth and are used to fill in where permanent teeth have been removed. Just like natural teeth, dentures need to be properly cared for. Use a gentle cleanser to brush your dentures, always keep them moist when they’re not in use, and be sure to keep your tongue and gums clean as well.
Extractions
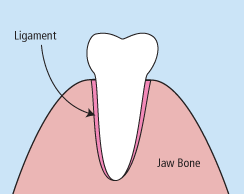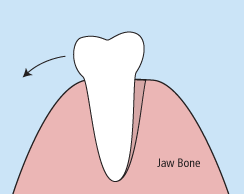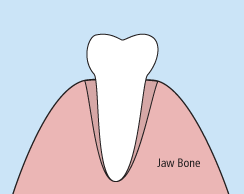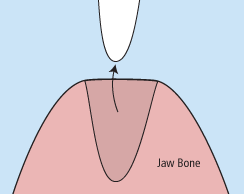 There are times when it is necessary to remove a tooth. Sometimes a baby tooth has misshapen or long roots that prevent it from falling out as it should, and the tooth must be removed to make way for the permanent tooth to erupt. At other times, a tooth may have so much decay that it puts the surrounding teeth at risk of decay, so your doctor may recommend removal and replacement with a bridge or implant. Infection, orthodontic correction, or problems with a wisdom tooth can also require removal of a tooth.
There are times when it is necessary to remove a tooth. Sometimes a baby tooth has misshapen or long roots that prevent it from falling out as it should, and the tooth must be removed to make way for the permanent tooth to erupt. At other times, a tooth may have so much decay that it puts the surrounding teeth at risk of decay, so your doctor may recommend removal and replacement with a bridge or implant. Infection, orthodontic correction, or problems with a wisdom tooth can also require removal of a tooth.
When it is determined that a tooth needs to be removed, your dentist may extract the tooth during a regular checkup or may request another visit for this procedure. The root of each tooth is encased within your jawbone in a “tooth socket,” and your tooth is held in that socket by a ligament. In order to extract a tooth, your dentist must expand the socket and separate the tooth from the ligament holding it in place. While this procedure is typically very quick, it is important to share with your doctor any concerns or preferences for sedation.
Once a tooth has been removed, neighboring teeth may shift, causing problems with chewing or with your jaw joint function. To avoid these complications, your dentist may recommend that you replace the extracted tooth.
Root Canals
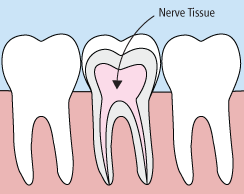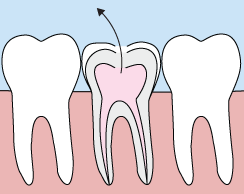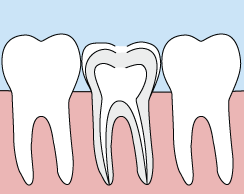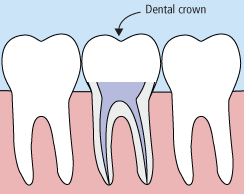 In the past, if you had a tooth with a diseased nerve, you'd probably lose that tooth. Today, with a special dental procedure called “root canal treatment,” your tooth can be saved. When a tooth is cracked or has a deep cavity, bacteria can enter the pulp tissue and germs can cause an infection inside the tooth. If left untreated, an abscess may form. If the infected tissue is not removed, pain and swelling can result. This can not only injure your jawbones, but it is also detrimental to your overall health.
In the past, if you had a tooth with a diseased nerve, you'd probably lose that tooth. Today, with a special dental procedure called “root canal treatment,” your tooth can be saved. When a tooth is cracked or has a deep cavity, bacteria can enter the pulp tissue and germs can cause an infection inside the tooth. If left untreated, an abscess may form. If the infected tissue is not removed, pain and swelling can result. This can not only injure your jawbones, but it is also detrimental to your overall health.
Root canal treatment involves one to three visits. During treatment, your general dentist or endodontist (a dentist who specializes in problems with the nerves of the teeth) removes the affected tissue. Next, the interior of the tooth will be cleaned and sealed. Finally, the tooth is filled with a dental composite. If your tooth has extensive decay, your doctor may suggest placing a crown to strengthen and protect the tooth from breaking. As long as you continue to care for your teeth and gums with regular brushing, flossing, and checkups, your restored tooth can last a lifetime.
Wisdom Teeth
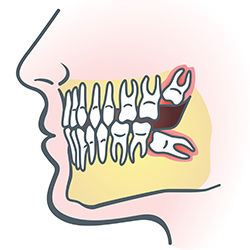 Wisdom teeth are types of molars found in the very back of your mouth. They usually appear in the late teens or early twenties, but may become impacted (fail to erupt) due to lack of room in the jaw or angle of entry. When a wisdom tooth is impacted, it may need to be removed. If it is not removed, you may develop gum tenderness, swelling, or even severe pain. Impacted wisdom teeth that are partially or fully erupted tend to be quite difficult to clean and are susceptible to tooth decay, recurring infections, and even gum disease.
Wisdom teeth are types of molars found in the very back of your mouth. They usually appear in the late teens or early twenties, but may become impacted (fail to erupt) due to lack of room in the jaw or angle of entry. When a wisdom tooth is impacted, it may need to be removed. If it is not removed, you may develop gum tenderness, swelling, or even severe pain. Impacted wisdom teeth that are partially or fully erupted tend to be quite difficult to clean and are susceptible to tooth decay, recurring infections, and even gum disease.
Wisdom teeth are typically removed in the late teens or early twenties because there is a greater chance that the teeth's roots have not fully formed and the bone surrounding the teeth is less dense. These two factors can make extraction easier as well as shorten the recovery time.
In order to remove a wisdom tooth, your dentist first needs to numb the area around the tooth with a local anesthetic. Since the impacted tooth may still be under the gums and imbedded in your jaw bone, your dentist will need to remove a portion of the covering bone to extract the tooth. In order to minimize the amount of bone that is removed with the tooth, your dentist will often “section” your wisdom tooth so that each piece can be removed through a small opening in the bone. Once your wisdom teeth have been extracted, the healing process begins. Depending on the degree of difficulty related to the extraction, healing time varies. Your dentist will share with you what to expect and provide instructions for a comfortable, efficient healing process.

 Website Powered by Sesame 24-7™
Website Powered by Sesame 24-7™